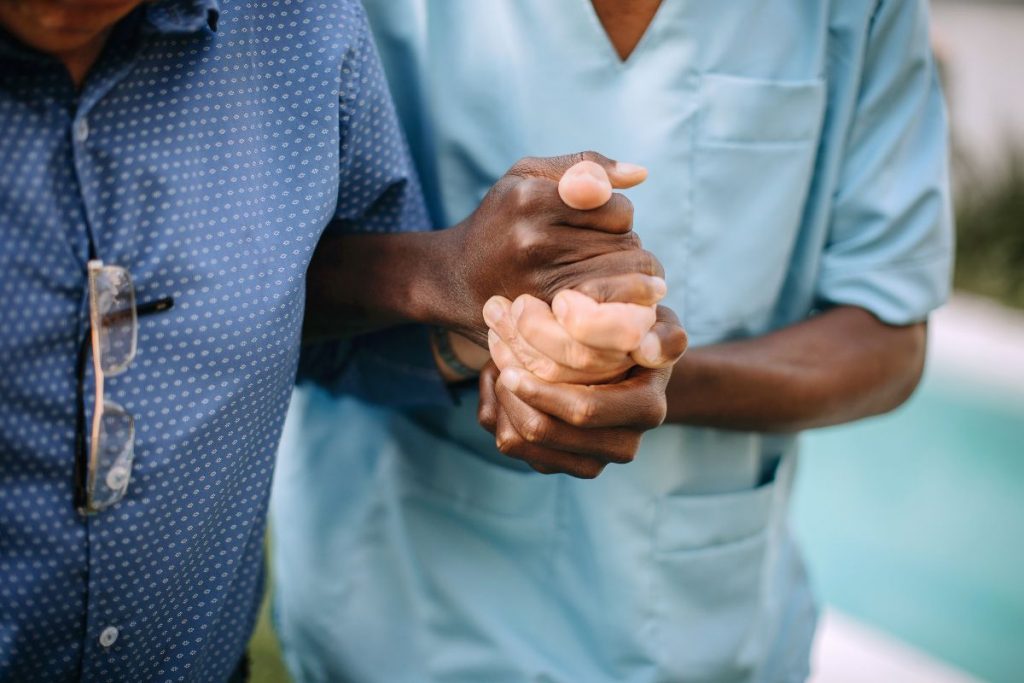
The federal Medicare program is not without its share of rules. The 3-day rule in Medicare is one that is often forgotten until it’s too late. Plus, it’s seen some significant changes in recent years. To avoid surprise medical bills, take a few minutes to learn what the 3-day rule is and how it applies to your Medicare coverage.
What Is a Skilled Nursing Facility?
A skilled nursing facility (SNF) provides care by registered nurses and other healthcare providers under a doctor’s supervision. It’s nearly the same level of care you’d get while in the hospital. Patients often go from the hospital to an SNF to continue recovering after a surgery, injury, or illness. In addition to nursing care, you may also get rehabilitation services like physical, speech, or occupational therapy.
Think of a skilled nursing facility as transitional care. The goal of an SNF is to give patients the care they need to heal and return home.

How Does the Skilled Nursing Facility 3-Day Rule Work?
To be eligible for services in a skilled nursing facility, Medicare beneficiaries must adhere to the 3-day rule. The rule states that you must have a qualified 3-day hospital stay before being transferred to an SNF. This stay can be in either a hospital or a critical access hospital (CAH) that has been approved to provide residents with swing bed services for acute care. No 3-day stay, no coverage.
Your transition to an SNF does not have to be right away. Coverage is extended to SNF services within 30 days of your hospital discharge, assuming your doctor deems skilled nursing care to be medically necessary.
Here’s where things get a little tricky. Those three days do not include any pre-admission time you might have spent in the emergency room, nor does any observation time count. Many people are surprised to find out that an overnight stay does not always mean you’ve become an inpatient. Your provider must officially admit you to the hospital before your 3-day stretch begins. Additionally, the day you are discharged does not count as one of those three days.
Fortunately for patients and their family members, the hospital should inform you of your eligibility if they intend to move you to a skilled nursing facility. The SNF itself should also verify your qualifying 3-day stay during the admission process. However, Medicare does not require skilled nursing facilities to give beneficiaries an Advance Beneficiary Notice of Non-Coverage (SNF ABN) if the 3-day requirement hasn’t been met. While not required, Medicare does strongly encourage facilities to make patients aware of this fact. If coverage isn’t available, patients must pay for extended care services out-of-pocket.
If you do qualify for SNF coverage, those benefits fall under Medicare Part A. Assuming you only have Original Medicare (Parts A and B), you’ll be responsible for the Part A deductible and cost-sharing amounts. In 2024, the Part A deductible is $1,632. Days 1-20 are covered at 100% by Medicare, and you’ll have a $204 copayment due each day. After the one-hundredth day, all costs are your responsibility, regardless of meeting the 3-day rule.
Get Help with Skilled Nursing Facility Costs
To find out more about skilled nursing facility coverage, talk to a Medicare advisor at Carolina Senior Benefits. Your advisor will help ensure you have the right plan for your needs. We’ll teach you about all your Medicare options and then help you enroll in the plans that make the most sense in your situation.
Reach out today to get started on your Medicare journey.